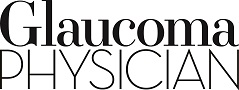Elevated intraocular pressure (IOP) remains the only modifiable risk factor in glaucoma,1-4 yet traditional tonometry provides only brief, office-based snapshots of a dynamic parameter. Traditional in-office measurement methods, such as Goldmann applanation tonometry (GAT), rebound tonometry, and dynamic contour tonometry (DCT), do not capture diurnal and nocturnal fluctuations that may contribute to optic nerve damage. Home tonometers enable intermittent self-monitoring but cannot reliably capture supine or nocturnal readings, limiting detection of early-morning spikes or abnormal circadian patterns.5 Patients with greater long-term IOP variability demonstrate faster visual field deterioration, underscoring the importance of comprehensive pressure assessment.6-13
Continuous monitoring technologies, including wearable contact lens–based sensors (CLBS) and implantable telemetric microelectro-mechanical systems (bioMEMS), facilitate round-the-clock tracking of diurnal and nocturnal IOP patterns. These devices offer the potential to detect previously unrecognized pressure peaks, guide individualized treatment targets, and inform management of patients with progressive glaucoma despite apparently controlled office readings. By capturing the full spectrum of IOP fluctuations, continuous monitoring may improve risk stratification and decision- making in treatment-resistant and normal-tension glaucoma.10
CLBS detect pressure-related changes at the ocular surface, whereas implantable devices measure IOP directly within the eye, potentially offering greater precision. Both approaches enable continuous assessment of IOP dynamics and generate longitudinal data that can support individualized treatment strategies.11,12
These devices employ pressure transducers based on piezoresistive, capacitive, optical, or microfluidic sensing mechanisms.14-16 Sensor components are typically fabricated from polymer, nanomaterial, or silicon-based substrates to optimize durability, sensitivity, and biocompatibility.17-19 The following sections summarize the mechanics of these technologies and the current clinical evidence for their use in continuous IOP monitoring.

Figure 1. A continuous intraocular pressure trace showing nocturnal peak and variability. From: Liu JH, Mansouri K, Weinreb RN. Estimation of 24-hour intraocular pressure peak timing and variation using a contact lens sensor. PLoS One. 2015;10(6):e0129529. Reprinted with permission.
Contact Lens–Based Sensors
Multiple studies have evaluated CLBS for continuous IOP monitoring. These devices detect pressure-related changes in corneal curvature using strain gauges, allowing assessment of dynamic IOP fluctuations based on associated radial stress and corneal flattening (increased pressure) or steepening (decreased pressure).20,21
The Sensimed Triggerfish is the most extensively studied CLBS and is approved for clinical use in the United States. Using a soft silicone contact lens with embedded strain gauges and microelectronics, Triggerfish enables noninvasive, continuous monitoring during normal daily activities and can capture diurnal and nocturnal IOP patterns not observed during office measurements (Figure 1). CLBS systems estimate IOP indirectly from corneal deformation measurements reported in millivolt equivalents rather than mmHg, limiting direct clinical interpretation because the relationship between corneal measurements and IOP is subtle, nonlinear, and influenced by corneoscleral biomechanics.22,23 Newer devices capable of reporting IOP in mmHg are under investigation.24,25
CLBS readings show reasonable correlation with standard tonometry methods, with most studies reporting values within ±5 mmHg of GAT and other modalities.26 CLBS tends to measure 2 to 3 mmHg higher than GAT but aligns more closely with DCT.26 Some variability exists, including evidence of measurement drift over time, though overall correlation with applanation tonometry remains moderate to excellent.27,28
CLBS devices are generally safe and well tolerated, with no serious adverse events reported. When worn continuously for 24 hours, common side effects include transient blurred vision, discomfort, conjunctival hyperemia, and mild worsening of ocular surface parameters, all typically resolving within 24 hours to a few days.26,29-32 Corneal erosions and increased superficial punctate keratitis have been reported, but all resolved within days, and no serious infectious events such as bacterial keratitis or corneal ulcers were documented.26,31 Patients should be counseled regarding these temporary, reversible symptoms.10
Implantable Sensors
Implantable bioMEMS-based sensors have been developed for continuous IOP monitoring from within the eye, with placement in the ciliary sulcus, anterior chamber, or suprachoroidal space. These devices enable long-term telemetric measurement but require surgical implantation. The Eyemate-IO system (Implandata Ophthalmic Products GmbH) is a capacitive pressure sensor implanted in the ciliary sulcus, typically during cataract surgery,33 whereas the smaller Eyemate-SC is placed in the suprachoroidal space for standalone glaucoma procedures.14
These capacitive sensors measure pressure by detecting changes in the distance between 2 plates via an electrical signal and consist of a hermetically sealed silicon-based sensor, integrated circuitry, and a metallic telemetry coil for wireless power and data transmission. Both devices are CE-marked in Europe but are not FDA-approved in the United States. Measurements are obtained using an external reader that wirelessly powers the implant and receives telemetric data. Early studies indicate acceptable safety, durability, and accuracy, supporting the feasibility of continuous absolute IOP monitoring, although implantation-related risks and long-term calibration remain limitations.10 Notably, Eyemate-IO measurements allow detailed assessment of diurnal patterns, with peak IOP and IOP variability associated with faster retinal nerve fiber layer thinning, whereas mean office IOP was not.35
Clinical evaluation of Eyemate-IO has demonstrated overall safety and feasibility. Long-term follow-up by Koutsonas et al. reported stable device performance over 37.5 months, but the first-generation ciliary sulcus implant was associated with pupillary distortion, occasional iris atrophy, measurement drift, and limited agreement with GAT.33 A second-generation sensor evaluated by Choritz et al showed improved biocompatibility and closer agreement with GAT, although readings remained approximately 3 mmHg higher.34 The suprachoroidal Eyemate-SC sensor has also demonstrated good safety and agreement with tonometry. Initial studies reported successful suprachoroidal implantation without migration or serious complications,36 with most measurements within ±5 mmHg of GAT after the early postoperative period.37 Follow-up of approximately 3 years confirmed device stability and consistent agreement with tonometry, supporting its use for long-term monitoring.38
Wearable CLBS and implantable bioMEMS devices provide complementary approaches to continuous monitoring. CLBS allow noninvasive 24-hour recording and can detect diurnal variation, nocturnal peaks, and ocular pulse–related signals associated with visual field progression.39 However, CLBS output does not directly correspond to mmHg, and correlation with tonometry is variable; transient ocular surface changes may also occur.40
Implantable sensors provide direct IOP measurement with stable long-term agreement with GAT but require intraocular surgery and may be associated with device-related complications or calibration drift. Overall, CLBS are useful for noninvasive assessment of circadian pressure patterns, whereas implantable sensors may be better suited for long-term monitoring in patients with progressive glaucoma who require precise, continuous IOP measurement.33-35

Clinical Utility and Integration into Glaucoma Care
Characterizing diurnal and nocturnal IOP patterns has important implications for treatment selection and optimization. Prostaglandin analogues, particularly bimatoprost and travoprost, provide the most consistent 24-hour IOP reduction, lowering both peak and trough pressures while reducing short-term variability.41,42 Several studies report greater daytime IOP reduction with evening dosing compared with morning administration in patients with primary open-angle glaucoma.43-46 Alpha-2 agonists and beta-blockers have similar overall IOP-lowering effects but reduced nocturnal efficacy,42,47,48 whereas carbonic anhydrase inhibitors appear to maintain better nighttime control.43,49,50 Fixed combinations, especially prostaglandin analogue–beta-blocker formulations, may provide the most stable 24-hour pressure profile. Knowledge of an individual’s circadian IOP pattern may therefore allow therapy to be tailored based on the timing and magnitude of pressure fluctuations.43
Some antiglaucoma medications, including timolol and apraclonidine, may develop tachyphylaxis with prolonged use, although the effect on long-term 24-hour control remains unclear.51-53 Surgical and laser interventions also influence IOP variability. Although selective laser trabeculoplasty (SLT) has not consistently altered overall 24-hour IOP patterns, its continuous effect on the trabecular meshwork may promote greater IOP stability.54 This may contribute to improved long-term disease control compared with initial topical therapy and reduce the need for incisional surgery, as documented in the LiGHT trial. In contrast, the episodic nature of medication use, particularly with suboptimal adherence, may limit control of IOP fluctuations.55 Trabeculectomy produces a greater reduction in diurnal variability than medical therapy in both primary open-angle and primary angle-closure glaucoma and has been associated with slower disease progression.9,56-59 Further studies are needed to assess the impact of tube shunts on IOP fluctuations and to compare their performance with trabeculectomy beyond mean IOP control.
Continuous IOP monitoring may further refine treatment selection by identifying nocturnal peaks, diurnal fluctuations, or inadequate medication response that may not be detected during office measurements. However, routine clinical use remains limited by technical challenges, including signal drift, telemetry complexity, and incomplete equivalence with standard mmHg-based tonometry.
Challenges and Limitations
Despite technological advances, clinical adoption of continuous IOP monitoring devices remains limited by device-specific constraints and patient selection criteria. Not all patients are suitable candidates for wearable or implantable systems. Self-tonometry requires training, reliable fixation, and proper technique, and measurements may be affected by corneal properties, limiting use in patients with corneal abnormalities. CLBS allow continuous monitoring but may cause ocular surface irritation, require strict lens hygiene, and in some cases require supervised use, which can limit routine clinical application.
Implantable bioMEMS sensors provide accurate, continuous IOP measurements but require intraocular implantation and are therefore best suited for selected patients. Surgical placement carries risks, including hyphema and device-related complications, and is generally restricted to eyes within a defined axial length range because of increased risk of pupillary block or surgical difficulty in very short (<22 mm) or long (>26 mm) eyes.33 Use in pediatric and young adult populations is also limited, particularly when combined with cataract surgery. Reported device-related effects include pupillary distortion, iris transillumination, and transient corneal decompensation, necessitating close postoperative monitoring. Ideal candidates are patients with glaucoma in whom continuous IOP monitoring is likely to meaningfully influence management—such as those with progression despite controlled office IOP—with current evidence supporting implantation at the time of nonpenetrating glaucoma surgery (NPGS). Conversely, implantation should be avoided in patients with contraindications to NPGS (eg, neovascular or angle-closure glaucoma), extreme refractive error (myopia > -6 D or hyperopia > +4 D) or axial length outside 22 to 26 mm, age <18 years, acute retinal detachment, uncontrolled diabetes with moderate-to-severe nonproliferative or proliferative diabetic retinopathy, the presence of another active implantable device in the head or neck, or intraoperative complications during NPGS (eg, trabeculo-Descemet membrane perforation).
Continuous monitoring also generates large volumes of data that require standardized processing, secure storage, and integration with electronic health records, raising concerns about interoperability, data privacy, and clinician workload. Device cost and unresolved medicolegal questions regarding responsibility for continuous data interpretation may further limit widespread use.
These technologies provide monitoring rather than treatment, and disease progression may still occur without appropriate pressure-lowering therapy. Continuous IOP assessment must therefore be combined with medical, laser, or surgical management. Future approaches may integrate monitoring with drug-delivery systems, including intraocular implants or contact lenses capable of controlled medication release.17,18
Future Directions and Research Priorities
Several next-generation technologies for continuous IOP monitoring are under development, with emphasis on sensor miniaturization to reduce ocular side effects and simplify implantation while maintaining measurement accuracy. Investigational approaches include interferometry-based systems and sensors incorporating novel materials, such as graphene, to improve durability and scalability. Corneal biomechanics may influence measurement accuracy, although advances in signal-processing algorithms may help compensate for these effects. Further clinical studies are needed to establish the safety, reliability, and clinical role of these emerging platforms.15,60-63
Conclusion
IOP remains the only modifiable risk factor in glaucoma, yet conventional tonometry provides only intermittent measurements of a dynamic parameter. Growing evidence suggests that circadian fluctuations, transient spikes, and long-term variability contribute to disease progression, particularly in patients who worsen despite controlled office IOP. Continuous monitoring technologies, including CLBS and implantable sensors, enable granular, longitudinal assessment of pressure patterns and may improve risk stratification and treatment selection. Early studies show promising safety and performance; however, clinical adoption is limited by challenges related to calibration, invasiveness, data interpretation, cost, and workflow integration. Further refinement and longitudinal outcome data are needed to define their role, though these technologies hold promise for more individualized, data-driven glaucoma care. GP
References
1. Weinreb RN, Khaw PT. Primary open-angle glaucoma. Lancet. 2004;363(9422):1711-1720. doi:10.1016/S0140-6736(04)16257-0
2. Weinreb RN, Aung T, Medeiros FA. The pathophysiology and treatment of glaucoma: a review. JAMA. 2014;311(18):1901-1911. doi:10.1001/jama.2014.3192
3. Goel M, Picciani RG, Lee RK, Bhattacharya SK. Aqueous humor dynamics: a review. Open Ophthalmol J. 2010;4:52-59. doi:10.2174/1874364101004010052
4. Kass MA, Heuer DK, Higginbotham EJ, et al. The Ocular Hypertension Treatment Study: a randomized trial determines that topical ocular hypotensive medication delays or prevents the onset of primary open-angle glaucoma. Arch Ophthalmol. 2002;120(6):701-830. doi:10.1001/archopht.120.6.701
5. Arora T, Bali SJ, Arora V, Wadhwani M, Panda A, Dada T. Diurnal versus office-hour intraocular pressure fluctuation in primary adult onset glaucoma. J Optom. 2015;8(4):239-243. doi:10.1016/j.optom.2014.05.005
6. Bhartiya S, Wadhwani M, Rai O, Patuel M, Dorairaj S, Sirish KN. Diurnal variation of IOP in angle closure disease: are we doing enough? Rom J Ophthalmol. 2019;63(3):208-216.
7. Cvenkel B, Atanasovska Velkovska M. Self-monitoring of intraocular pressure using Icare HOME tonometry in clinical practice. Clin Ophthalmol. 2019;13:841-847. doi:10.2147/OPTH.S198846
8. Quaranta L, Katsanos A, Russo A, Riva I. 24-hour intraocular pressure and ocular perfusion pressure in glaucoma. Surv Ophthalmol. 2013;58(1):26-41. doi:10.1016/j.survophthal.2012.05.003
9. Hong S, Seong GJ, Hong YJ. Long-term intraocular pressure fluctuation and progressive visual field deterioration in patients with glaucoma and low intraocular pressures after a triple procedure. Arch Ophthalmol. 2007;125(8):1010-1013. doi:10.1001/archopht.125.8.1010
10. Monsálvez-Romín D, Martínez-Albert N, García-Domene MC, Ortí-Navarro S. Current and emerging technologies for continuous intraocular pressure monitoring in the control of glaucoma progression: a scoping review. J Clin Med. 2025;14(24):8795. doi:10.3390/jcm14248795
11. Raveendran R, Prabakaran L, Senthil R, et al. Current innovations in intraocular pressure monitoring biosensors for diagnosis and treatment of glaucoma—novel strategies and future perspectives. Biosensors (Basel). 2023;13(6):663. doi:10.3390/bios13060663
12. Sanchez I, Martin R. Advances in diagnostic applications for monitoring intraocular pressure in glaucoma: a review. J Optom. 2019;12(4):211-221. doi:10.1016/j.optom.2018.12.003
13. Konstas AG, Kahook MY, Araie M, et al. Diurnal and 24-h intraocular pressures in glaucoma: monitoring strategies and impact on prognosis and treatment. Adv Ther. 2018;35(11):1775-1804. doi:10.1007/s12325-018-0812-z
14. Abhinav V, Basu P, Verma SS, et al. Advancements in wearable and implantable BioMEMS devices: transforming healthcare through technology. Micromachines (Basel). 2025;16(5):522. doi:10.3390/mi16050522
15. Wu KY, Mina M, Carbonneau M, Marchand M, Tran SD. Advancements in wearable and implantable intraocular pressure biosensors for ophthalmology: a comprehensive review. Micromachines (Basel). 2023;14(10):1915. doi:10.3390/mi14101915
16. Yang C, Huang X, Li X, et al. Wearable and implantable intraocular pressure biosensors: recent progress and future prospects. Adv Sci (Weinh). 2021;8(6):2002971. doi:10.1002/advs.202002971
17. Fardoost A, Karimi K, Singh J, Patel H, Javanmard M. Enhancing glaucoma care with smart contact lenses: an overview of recent developments. Biomed Microdevices. 2025;27(2):18. doi:10.1007/s10544-025-00740-7
18. Khosravi A, Zarepour A, Zarrabi A, Iravani S. MXene-based wearable contact lenses: integrating smart technology into vision care. Nanomicro Lett. 2025;18(1):20. doi:10.1007/s40820-025-01863-5
19. Kazanskiy NL, Khonina SN, Butt MA. Smart contact lenses-a step towards non-invasive continuous eye health monitoring. Biosensors (Basel). 2023;13(10):933. doi:10.3390/bios13100933
20. Shi Y, Jiang N, Bikkannavar P, Cordeiro MF, Yetisen AK. Ophthalmic sensing technologies for ocular disease diagnostics. Analyst. 2021;146(21):6416-6444. doi:10.1039/d1an01244d
21. Shin H, Seo H, Chung WG, Joo BJ, Jang J, Park JU. Recent progress on wearable point-of-care devices for ocular systems. Lab Chip. 2021;21(7):1269-1286. doi:10.1039/d0lc01317j
22. Wei Y, Zhang Y, Chen Z, et al. A novel contact lens sensor system for continuous intraocular pressure monitoring: evaluation of accuracy in human eyes. Ophthalmol Sci. 2025;5(5):100826. doi:10.1016/j.xops.2025.100826
23. Dunbar GE, Shen BY, Aref AA. The Sensimed Triggerfish contact lens sensor: efficacy, safety, and patient perspectives. Clin Ophthalmol. 2017;11:875-882. doi:10.2147/OPTH.S109708
24. Zhang Y, Wei Y, Lee CHC, et al. Continuous 24-hour intraocular pressure monitoring in normal Chinese adults using a novel contact lens sensor system. Br J Ophthalmol. 2024;108(11):1535-1542. doi:10.1136/bjo-2023-323361
25. Zhang Y, Yang W, Chen Z, et al. Continuous intraocular pressure variations following positional transitions in normal subjects and open angle glaucoma patients using a contact lens sensor system. Graefes Arch Clin Exp Ophthalmol. 2025;263(4):1061-1070. doi:10.1007/s00417-024-06680-x
26. Wasilewicz R, Varidel T, Simon-Zoula S, Schlund M, Cerboni S, Mansouri K. First-in-human continuous 24-hour measurement of intraocular pressure and ocular pulsation using a novel contact lens sensor. Br J Ophthalmol. 2020;104(11):1519-1523. doi:10.1136/bjophthalmol-2019-315276
27. Gillmann K, Wasilewicz R, Hoskens K, Simon-Zoula S, Mansouri K. Continuous 24-hour measurement of intraocular pressure in millimeters of mercury (mmHg) using a novel contact lens sensor: Comparison with pneumatonometry. PLoS One. 2021;16(3):e0248211. doi:10.1371/journal.pone.0248211
28. Beltran-Agulló L, Buys YM, Jahan F, et al. Twenty-four hour intraocular pressure monitoring with the Sensimed Triggerfish contact lens: effect of body posture during sleep. Br J Ophthalmol. 2017;101(10):1323-1328. doi:10.1136/bjophthalmol-2016-308710
29. Otsuka M, Hayashi A, Tojo N. Questionnaire survey on complications during 24-h measurement of intraocular pressure-related patterns with a contact lens sensor. Int Ophthalmol. 2020;40(8):1963-1968. doi:10.1007/s10792-020-01370-z
30. Zhang Y, Wei Y, Karunaratne IK, et al. A new contact lens sensor system for continuous intraocular pressure monitoring: evaluation of safety and tolerability. Eye Contact Lens. 2022;48(10):439-444. doi:10.1097/ICL.0000000000000926
31. Huang SK, Ishii M, Mizuki Y, et al. Circadian fluctuation changes in intraocular pressure measured using a contact lens sensor in patients with glaucoma after the adjunctive administration of ripasudil: a prospective study. J Pers Med. 2023;13(5):800. doi:10.3390/jpm13050800
32. Carnero E, Bragard J, Urrestarazu E, et al. Continuous intraocular pressure monitoring in patients with obstructive sleep apnea syndrome using a contact lens sensor. PLoS One. 2020;15(3):e0229856. doi:10.1371/journal.pone.0229856
33. Koutsonas A, Walter P, Roessler G, Plange N. Long-term follow-up after implantation of a telemetric intraocular pressure sensor in patients with glaucoma: a safety report. Clin Exp Ophthalmol. 2018;46(5):473-479. doi:10.1111/ceo.13100
34. Choritz L, Mansouri K, van den Bosch J, et al. Telemetric measurement of intraocular pressure via an implantable pressure sensor—12-month results from the ARGOS-02 trial. Am J Ophthalmol. 2020;209:187-196. doi:10.1016/j.ajo.2019.09.011
35. Micheletti E, Rao H, Weinreb RN, Mansouri K; EYEMATE-IO study group. Intraocular pressure monitoring using an implantable sensor detects structural glaucoma progression in the EYEMATE-IO trial. Am J Ophthalmol. 2025;277:112-119. doi:10.1016/j.ajo.2025.05.010
36. Szurman P, Mansouri K, Dick HB, et al. Safety and performance of a suprachoroidal sensor for telemetric measurement of intraocular pressure in the EYEMATE-SC trial. Br J Ophthalmol. 2023;107(4):518-524. doi:10.1136/bjophthalmol-2021-320023
37. Szurman P, Gillmann K, Seuthe AM, et al. EYEMATE-SC trial: twelve-month safety, performance, and accuracy of a suprachoroidal sensor for telemetric measurement of intraocular pressure. Ophthalmology. 2023;130(3):304-312. doi:10.1016/j.ophtha.2022.09.021
38. Micheletti E, Mansouri K, Dick HB, et al. Long-term safety and performance of a suprachoroidal pressure sensor system: results of the EYEMATE-SC trial follow-up study. Ophthalmology. 2025;132(7):775-784. doi:10.1016/j.ophtha.2025.01.021
39. Kim YW, Kim JS, Lee SY, et al. Twenty-four-hour intraocular pressure-related patterns from contact lens sensors in normal-tension glaucoma and healthy eyes: the Exploring Nyctohemeral Intraocular pressure–related pattern for Glaucoma Management (ENIGMA) study. Ophthalmology. 2020;127(11):1487-1497. doi:10.1016/j.ophtha.2020.05.010
40. Morales-Fernandez L, Garcia-Bella J, Martinez-de-la-Casa JM, et al. Changes in corneal biomechanical properties after 24 hours of continuous intraocular pressure monitoring using a contact lens sensor. Can J Ophthalmol. 2018;53(3):236-241. doi:10.1016/j.jcjo.2017.10.028
41. Mansouri K, Weinreb RN, Medeiros FA. Is 24-hour intraocular pressure monitoring necessary in glaucoma? Semin Ophthalmol. 2013;28(3):157-164. doi:10.3109/08820538.2013.771201
42. Stewart WC, Konstas AG, Nelson LA, Kruft B. Meta-analysis of 24-hour intraocular pressure studies evaluating the efficacy of glaucoma medicines. Ophthalmology. 2008;115(7):1117-1122.e1. doi:10.1016/j.ophtha.2007.10.004
43. Konstas AG, Quaranta L, Bozkurt B, et al. 24-h Efficacy of Glaucoma Treatment Options. Adv Ther. 2016;33(4):481-517. doi:10.1007/s12325-016-0302-0
44. Konstas AG, Nakos E, Tersis I, Lallos NA, Leech JN, Stewart WC. A comparison of once-daily morning vs evening dosing of concomitant latanoprost/timolol. Am J Ophthalmol. 2002;133(6):753-757. doi:10.1016/s0002-9394(02)01460-5
45. Konstas AG, Katsanos A, Quaranta L, Mikropoulos DG, Tranos PG, Teus MA. Twenty-four hour efficacy of glaucoma medications. Prog Brain Res. 2015;221:297-318. doi:10.1016/bs.pbr.2015.06.010
46. Konstas AG, Maltezos AC, Gandi S, Hudgins AC, Stewart WC. Comparison of 24-hour intraocular pressure reduction with two dosing regimens of latanoprost and timolol maleate in patients with primary open-angle glaucoma. Am J Ophthalmol. 1999;128(1):15-20. doi:10.1016/s0002-9394(99)00073-2
47. Seibold LK, DeWitt PE, Kroehl ME, Kahook MY. The 24-hour effects of brinzolamide/brimonidine fixed combination and timolol on intraocular pressure and ocular perfusion pressure. J Ocul Pharmacol Ther. 2017;33(3):161-169. doi:10.1089/jop.2016.0141
48. Konstas AG, Mikropoulos D, Kaltsos K, Jenkins JN, Stewart WC. 24-hour intraocular pressure control obtained with evening- versus morning-dosed travoprost in primary open-angle glaucoma. Ophthalmology. 2006;113(3):446-450. doi:10.1016/j.ophtha.2005.10.053
49. Sit AJ. Intraocular pressure variations: causes and clinical significance. Can J Ophthalmol. 2014;49(6):484-488. doi:10.1016/j.jcjo.2014.07.008
50. Cheng JW, Cheng SW, Gao LD, Lu GC, Wei RL. Intraocular pressure–lowering effects of commonly used fixed-combination drugs with timolol: a systematic review and meta-analysis. PLoS One. 2012;7(9):e45079. doi:10.1371/journal.pone.0045079
51. Thelen U, Schnober D, Schölzel S, et al. Long-term cost and efficacy analysis of latanoprost versus timolol in glaucoma patients in Germany. Int J Ophthalmol. 2013;6(2):155-159. doi:10.3980/j.issn.2222-3959.2013.02.09
52. Novack GD, O’Donnell MJ, Molloy DW. New glaucoma medications in the geriatric population: efficacy and safety. J Am Geriatr Soc. 2002;50(5):956-962. doi:10.1046/j.1532-5415.2002.50226.x
53. Tătaru CP, Purcărea VL. Antiglaucoma pharmacotherapy. J Med Life. 2012;5(3):247-251.
54. Tojo N, Oka M, Miyakoshi A, Ozaki H, Hayashi A. Comparison of fluctuations of intraocular pressure before and after selective laser trabeculoplasty in normal-tension glaucoma patients. J Glaucoma. 2014;23(8):e138-e143. doi:10.1097/IJG.0000000000000026
55. Gazzard G, Konstantakopoulou E, Garway-Heath D, et al. Laser in Glaucoma and Ocular Hypertension (LiGHT) trial: six-year results of primary selective laser trabeculoplasty versus eye drops for the treatment of glaucoma and ocular hypertension. Ophthalmology. 2023;130(2):139-151. doi:10.1016/j.ophtha.2022.09.009
56. Matsuoka M, Ando A, Minamino K, et al. Dampening of diurnal intraocular pressure fluctuation by combined trabeculotomy and sinusotomy in eyes with open-angle glaucoma. J Glaucoma. 2013;22(4):290-293. doi:10.1097/IJG.0b013e31824479e6
57. Liang YB, Xie C, Meng HL, et al. Daytime fluctuation of intraocular pressure in patients with primary angle-closure glaucoma after trabeculectomy. J Glaucoma. 2013;22(5):349-354. doi:10.1097/IJG.0b013e31826a7dd5
58. Bhartiya S, Ichhpujani P. The need to maintain intraocular pressure over 24 hours. J Curr Glaucoma Pract. 2012;6(3):120-123. doi:10.5005/jp-journals-10008-1118
59. Medeiros FA, Weinreb RN, Zangwill LM, et al. Long-term intraocular pressure fluctuations and risk of conversion from ocular hypertension to glaucoma. Ophthalmology. 2008;115(6):934-940. doi:10.1016/j.ophtha.2007.08.012
60. Li Y, Li L, Ye Z, et al. A novel implantable piezoresistive microsensor for intraocular pressure measurement. ACS Sens. 2024;9(8):3958-3966. doi:10.1021/acssensors.4c00705
61. Bhamra H, Tsai JW, Huang YW, Yuan Q, Shah JV, Irazoqui P. A subcubic millimeter wireless implantable intraocular pressure monitor microsystem. IEEE Trans Biomed Circuits Syst. 2017;11(6):1204-1215. doi:10.1109/TBCAS.2017.2755596
62. Xu X, Liu Z, Wang L, Huang Y, Yang H. High-accuracy film-integrated optical sensor for real-time intraocular pressure monitoring. Micromachines (Basel). 2023;14(2):353. doi:10.3390/mi14020353
63. Xu J, Cui T, Hirtz T, et al. Highly transparent and sensitive graphene sensors for continuous and noninvasive intraocular pressure monitoring. ACS Appl Mater Interfaces. 2020;12(16):18375-18384. doi:10.1021/acsami.0c02991
64. Liu JH, Mansouri K, Weinreb RN. Estimation of 24-hour intraocular pressure peak timing and variation using a contact lens sensor. PLoS One. 2015;10(6):e0129529. doi:10.1371/journal.pone.0129529